A car crash can change your life in seconds — but you don’t have to face recovery alone. If your auto insurance claim is denied, it can feel like another blow. Yet you still have rights under Texas law to challenge that denial and seek fair compensation. Under Texas Civil Practice & Remedies Code Chapters 33 & 41, you can hold negligent parties accountable and, if your insurer acts in bad faith, pursue additional damages. Whether you were hurt in a car accident, truck accident, or facing delays in a wrongful death compensation claim, these steps will guide you through the auto insurance claim denial process with confidence.
These steps protect your rights under Texas law from the first notice.
Summary Of Immediate Actions
Before diving into the details, here’s a snapshot of the moves you can’t afford to miss—and when to hit them.
| Action | Why It Matters | Deadline |
|---|---|---|
| Review Denial Notice | Pinpoints the insurer’s exact objections and any errors. | 30–60 days (typically) |
| Gather Documentation | Builds the factual backbone of your challenge. | ASAP |
| File Internal Appeal | Forces a fresh look at procedural mistakes. | Per your policy window |
Keep this table handy. It’s your cheat sheet for acting fast and staying organized.
Essential Moves After Claim Denial
• Pinpoint Denial Reasons
Crack open that denial letter and underline the insurer’s logic. Look for mix-ups—wrong claim numbers, missing pages, or inaccurate dates.
• Track Your Deadlines
Under Texas Insurance Code Chapter 41, most appeals land in the 30–60 day window. Mark your calendar the moment you see the denial.
• Assemble Core Evidence
Pull together medical bills, repair estimates, police reports, photographs, and witness statements—everything that tells your story.
• Craft A Targeted Internal Appeal
Address each denial point one by one. Attach your evidence in a clear, labeled order so nothing gets overlooked.
• Escalate If Needed
If your appeal stalls, ask for an independent review or reach out to a Houston car accident lawyer who knows the ropes.
Key Takeaway
A prompt, methodical response can turn a denial into an approval.
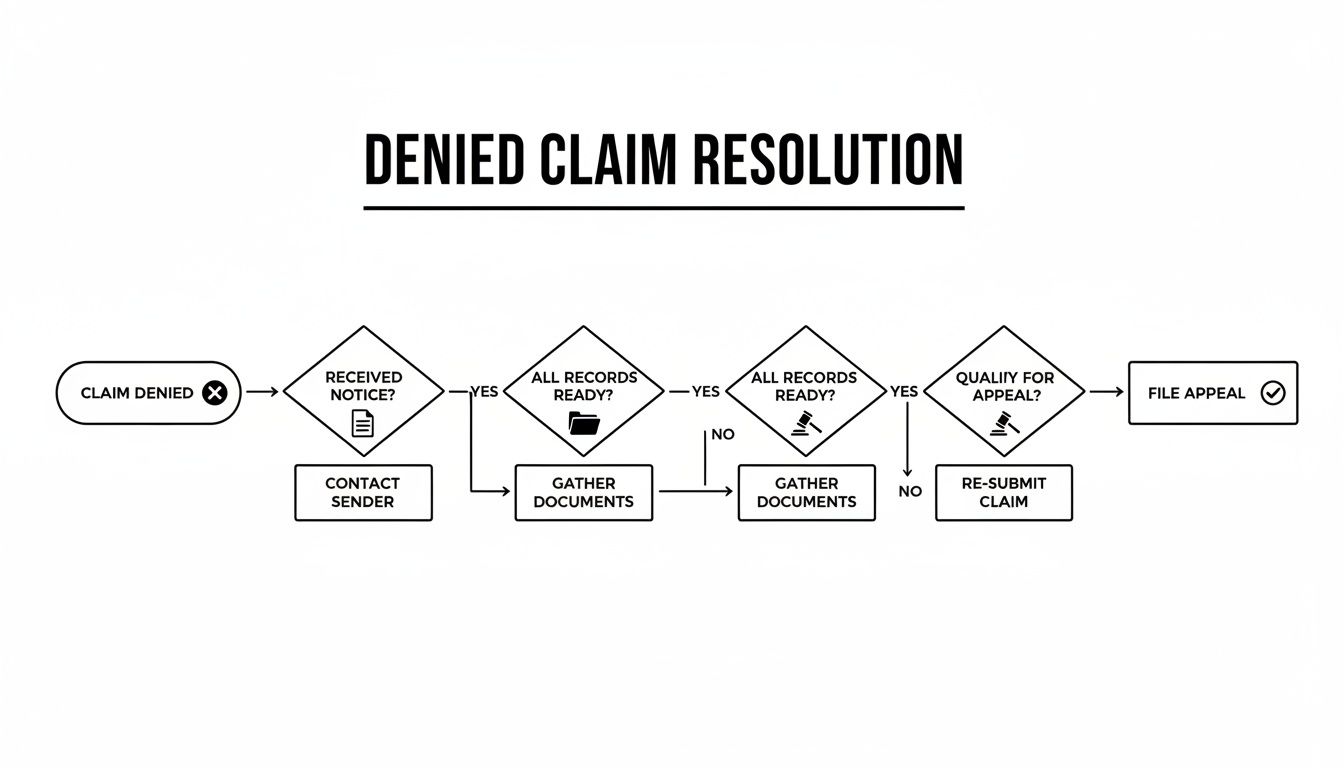
This infographic lays out the decision tree you’ll follow after a denial. It shows how sticking to Notice, Records, and Appeals steps keeps all your options alive.
Organizing Your Appeal
Every phone call, email, and letter deserves its own date stamp. A simple spreadsheet or a dedicated folder can make all the difference. When you compile your appeal packet, label each document—“Medical Bill – Dr. Smith 1/15/24,” “Repair Estimate – Joe’s Garage 2/03/24,” and so on.
Clarity is power. Insurers are more likely to concede when your facts are easy to digest. If internal channels drag, start drafting your complaint to the Texas Department of Insurance right away.
When To Seek Help
If you’re still hitting a wall—or your losses outstrip policy limits—talk to a Texas injury attorney. Under Texas Civil Practice & Remedies Code Chapters 33 and 41, a lawyer can help you file bad-faith claims or pursue litigation. That step can protect your rights and push for a fair recovery.
Understanding The Denial Notice
When you open that denial notice, think of it as the insurer’s road map showing exactly why your auto insurance claim hit a dead end. Read every line—this is where you’ll find the clues you need to fight back.
Common Reasons Behind A Denial
- Procedural Errors: Wrong claim number, missed deadline, or simple typo.
- Missing Documentation: No medical bills, repair invoices, or police reports on file.
- Coverage Exclusions: Specific policy clauses that bar certain types of damage.
- Pre-Existing Conditions: The insurer insists your current injury predates the accident.
Take, for example, a Houston driver rear-ended on I-45 who discovered a tiny exclusion for aftermarket parts tucked into their policy. Suddenly, the bill for upgraded bumpers and lights wasn’t covered—and the denial notice spelled it out in black and white.
Texas imposes strict deadlines, too. Under Texas Civil Practice & Remedies Code Chapter 16, you generally have two years to file suit after a denial. Miss that window, and you’ve lost your chance—comparing fault only weakens claims if you share blame in the crash.
Decoding Liability And Fault
Liability answers one simple question: who pays when damage happens? In Texas, the at-fault driver covers injuries and property losses. If you’re partly at fault, comparative fault kicks in and reduces your award by your percentage of blame.
Imagine you’re assigned 10% fault on a $10,000 recovery. The insurer will cut your check for $9,000. It may feel like splitting hairs, but understanding these mechanics makes a heavy denial letter far less daunting.
Key Insight
Policy language can sound like Latin. Circle words like liability, damages, and comparative fault so you know exactly what’s being argued.
Next, it’s time to hunt for hidden exclusions. Insurers often define “damages” narrowly—only certain medical bills, repair costs, or pain-and-suffering awards qualify.
| Term | Plain-English Meaning |
|---|---|
| Liability | Who’s legally responsible |
| Comparative Fault | Your percentage of blame |
| Damages | Funds to cover your losses |
| Statute of Limitations | Deadline to file suit |
Once you map those definitions onto your denial notice, each objection snaps into focus—no more guessing games.
Next Steps After Decoding Notice
Now that you’ve unraveled the insurer’s logic, lay out a clear action plan:
- List each denial reason and pair it with your supporting documents.
- Identify missing items—medical records, repair estimates, police reports.
- Pull together bills or expert opinions to challenge cost-based exclusions.
- Schedule follow-up calls before Texas Department of Insurance deadlines.
Keep a simple log—date, time, who you spoke with—and you’ll have a rock-solid trail for regulators or your lawyer. With these pieces in place, you’re ready to launch an internal appeal or take the dispute external.
Understanding every line of that denial notice isn’t just busywork. It’s how you turn confusion into leverage and breathe real life into your claim.
Navigating The Internal Appeal Process
An internal appeal often makes sense as your first move when an insurer turns down your claim. Believe it or not, simple mistakes—like missing documentation or incorrect claim numbers—show up in about 19% of denials. Fixing those errors leads to success nearly 44% of the time.
That insight comes from a 2025 industry analysis by Talli, which found procedural hiccups far more common than true coverage gaps. For the full breakdown, check out their report at blog.talli.ai.

Appeal Deadlines In Texas
Most Texas policies give you 30 to 60 days after denial to file internally. As soon as you receive that letter, block out those dates on your calendar.
- Document each deadline to stay on track.
- Link every piece of evidence to its submission date.
- Mail your appeal via certified mail or use the insurer’s secure portal.
Gathering Persuasive Evidence
Your appeal lives or dies on the strength of your proof. Start with medical records, repair estimates, and any missing X-ray images.
Then round up witness statements and clear photos of the scene.
Example: A Houston driver lost coverage for a back injury—until missing X-ray scans surfaced in the appeal packet and overturned the denial.
Drafting A Focused Appeal Letter
Think of your appeal letter as a roadmap through the insurer’s objections. Open with your name, policy number, and claim details. Then:
- Use headings that mirror the denial notice.
- Address each reason for denial in its own paragraph.
- Attach evidence labels (for example, “X-ray – 2/15/24”) right where you reference them.
Counter common defenses by quoting your policy language or accepted medical guidelines.
Follow-Up And Tracking Strategy
Once your packet is off to the insurer, keep a running log of every call, email, or chat. Ask for a reference number—and the rep’s name—each time you reach out.
- Hold on to your certified mail receipts as proof of timely filing.
- Send polite check-in emails if two weeks pass with no response.
- If delays drag on, write a brief note to a supervisor or the compliance department.
For more on handling adjusters, see our guide on how to deal with insurance adjusters.
Sample Defense Counter Language
| Insurer Defense | Sample Counter Language |
|---|---|
| Missing X-ray | “Attached X-ray dated 2/15/24 confirms injury severity.” |
| Policy Exclusion | “Section IV A covers this treatment without exclusion.” |
Tailor each phrase to your policy’s exact wording and your assembled evidence.
Keeping Your Appeal On Track
Set calendar alerts for two weeks before every deadline. When things stall, request a written status update.
- Use one folder—physical or digital—for all appeal documents.
- Jot down any commitments or turnaround times the insurer mentions.
- Prepare to push for an external review if this internal step falls short.
A well-organized appeal often flips an initial denial into an approval—saving you time and stress.
When To Consider Legal Help
If you hit another roadblock—or if insurer tactics feel shady—it might be time to talk with a lawyer. A Texas injury attorney can:
- Evaluate repeated technical denials.
- Decode vague or overbroad coverage defenses.
- Advise on bad-faith claims under the Texas Civil Practice & Remedies Code.
- Watch for looming statute-of-limitations deadlines or fresh evidence.
Our Houston car accident team offers free consultations to review your appeal packet and map out next steps.
Checklist For A Strong Internal Appeal
- Notice letter with denial dates and codes
- Policy declarations and relevant coverage excerpts
- Chronological timeline of incident and treatment
- All medical bills, X-rays, and repair invoices
- Witness statements with contact details
- Detailed appeal letter with numbered sections
- Proof of certified mailing or portal confirmations
Keep this list handy to ensure nothing slips through the cracks.
Moving Beyond Internal Appeals
If your insurer still says “no,” the next stop is the Texas Department of Insurance. They can:
- Investigate procedural errors you’ve documented
- Escalate your case to an independent review under ACA rules
When filing your complaint, include:
- A clear reference to your internal appeal
- Copies of every letter, form, and correspondence
- Notes on any financial or health harm from delays
A thorough, well-timed internal appeal under Texas rules often paves the way for a favorable outcome—or gives you the evidence needed for the next phase.
Gathering Evidence And Documentation
Putting together a rock-solid appeal means having every piece of your story at your fingertips. Start by pulling every document tied to the crash: medical charts, bills, repair estimates, police records, and any witness notes.
Building A Clear Timeline
Mapping out each event—from the moment of impact to every doctor’s appointment—brings clarity. I recommend a simple tracker with columns for Date, Description, Document Link, and Coverage Clause so nothing slips through the cracks.
- Date
- Document Type
- Source Name
- Coverage Clause
- File Location
| Document Type | Purpose |
|---|---|
| Medical Record | Prove injury severity and treatment path |
| Repair Estimate | Validate property damage costs |
| Police Report | Show official accident findings |
| Witness Statement | Support liability and fault analysis |
This numbered system makes citing evidence in your appeal nearly foolproof.
Labeling And Organizing Files
Chaos kills a claim. I’ve seen insurers reject appeals simply because they couldn’t find the right invoice. Color-code folders—digital or physical—and keep consistent naming across every file.
• Label like “Doc23_Medical_1-15-24”
• Store copies in a shared cloud drive with read-only access
• Archive originals offline to prevent accidental edits
Attorney Bryan Fagan emphasizes simplicity:
Expert Insight
Clear labels and simple folder trees cut review time in half.
Case Study In Effective Documentation
Consider a client rear-ended on Loop 610. Their initial appeal missed a repair invoice—and the insurer said no. Once that invoice landed in a “Repairs_03-05-24” folder, the denial flipped to approval within days.
Reviewing Medical Records And Bills
Don’t assume your records arrive complete. Order full charts from every provider, then audit them:
• Look for missing dates or unsigned notes
• Verify provider details (NPI numbers, addresses) match your policy
• Cross-check billed amounts against the insurer’s fee schedule
Catching duplicate charges or non-covered services early avoids nasty surprises.
Collecting Repair Documents
Never settle on a single estimate. I always advise clients to get at least two quotes and keep every receipt:
• Snap clear before-and-after photos of damage
• Log your vehicle’s mileage to prove consistent use
• Save detailed invoices that break down parts and labor
This level of proof cements any property damage claim.
Leveraging Automation And AI
When insurers dig in, tech can be your secret weapon. OCR scanners and claims-management tools reveal missing dates or policy-code mismatches in seconds.
• Auto-flag incomplete forms or incorrect fields
• Extract text from images and PDFs instantly
• Highlight discrepancies before you hit send
41% of providers now face 10% or higher denial rates, but among the 14% using AI, 69% report reduced denials and faster resubmissions—trimming manual review time by up to 50%. Discover more insights about healthcare claim denials on Experian.
Linking Evidence To Coverage
Every file should point back to a specific policy clause. I jot a quick note next to each document:
• “Covers emergency treatment under Section IV.A”
• Highlight total-loss or out-of-pocket limits
• Flag exclusions so you can address them head-on
Finish with a master checklist in your spreadsheet, ticking off each item against your policy language.
For a deep dive into police reports and deadlines, check out our guide on filing an accident report in Houston, TX.
With this organized evidence package, you’ll step into your appeal—or regulator complaint—with confidence.
Filing External Complaints And Seeking Additional Aid

When your insurer still says no after an internal appeal, it’s time to widen the net. State and federal agencies can step in. You’ll see how to lodge a Texas Department of Insurance complaint, request an independent review, and tap into patient assistance programs. Follow along to stay organized—and in control—when your claim hits a wall.
Filing A Complaint With Texas Department Of Insurance
Texas law gives you the right to ask the Texas Department of Insurance (TDI) to look into unfair denials. They’ll examine the paperwork, spot any procedural slip-ups, and even mediate between you and your insurer. To get started, gather your appeal letters, policy excerpts, and a clear timeline of what happened.
| Action | Why It Matters | Deadline |
|---|---|---|
| Complete TDI Complaint Form | Alerts regulators to unfair denials | Within 1 year of denial |
| Attach Internal Appeal Documents | Shows insurer had a chance to fix errors | At filing time |
| Provide Evidence Of Harm | Illustrates real loss from the denial | At filing time |
Once TDI has your packet, they’ll assign an investigator. Sometimes a quick mediation uncovers missing paperwork or a simple misinterpretation—and gets your claim back on track.
Requesting Independent External Review
If you’re on an ACA marketplace plan or an ERISA-regulated employer plan, an independent review might be your next move. This brings in a neutral examiner to reassess coverage disputes—especially critical when insurers deny new or experimental treatments.
To be eligible, your policy must:
- Be an ACA marketplace or ERISA employer plan
- Have exhausted the internal appeal process
- Not already be in litigation
Mail your request to the address in your denial letter or grab the forms at Healthcare.gov. Standard reviews wrap up in 45 days, and urgent cases can finish in 72 hours.
Key Insight
Independent reviewers overturn about 33% of coverage denials nationwide.
Exploring Patient Assistance Programs
Denied benefits don’t have to mean going without. Patient assistance programs can fill the gap. Last year, 54% of commercially insured adults saw medication coverage denied. Linking appeals with aid from drug manufacturers (43%) or charitable foundations (40%) often tips the scales.
Look into:
- Manufacturer assistance for brand-name drugs
- National or local charitable foundations
- Hospital-based aid programs and community health centers
Case In Point
A Dallas driver was refused coverage for a vital heart medication. Within weeks of applying to the drug maker’s assistance program—and including her appeal documents—she regained access to her treatment.
Documenting Health And Financial Harm
Your complaint gains real weight when you show documented losses. Start a simple journal to note health setbacks and unexpected bills. Gather receipts, mileage logs, and medical notes to paint a full picture of what you’ve endured.
• Save all pharmacy receipts and co-pays
• Ask providers for letters on harm caused by treatment delays
• Keep bank statements highlighting extra expenses
“Linking financial aid applications with appeals creates leverage insurers can’t ignore.”
By detailing both health setbacks and out-of-pocket hits, you make every external complaint or review more compelling.
Sample Complaint Form Templates
Pre-filled forms take the guesswork out of filing. Download the TDI complaint form and an ACA external review template. Then:
- Fill in your specifics
- Attach supporting documents
- Submit via certified mail or secure portal
A clear template helps you avoid costly omissions.
Tracking Deadlines And Follow-Up
Missing a deadline can derail your entire effort. Build a date-stamped log, set calendar reminders, and hold onto certified mail receipts. As each deadline approaches, send a polite status inquiry to keep your case top of mind. Detailed records show agencies—and your lawyer—just how proactive you’ve been.
When To Seek Legal Assistance
Sometimes even external routes hit a dead end. If denials persist, a Texas attorney experienced in insurance disputes can step in. Under Texas Civil Practice & Remedies Code Chapters 33 and 41, you may pursue bad-faith damages if your insurer unreasonably delays or denies payment.
A lawyer can:
- Draft a precise bad-faith demand letter
- Quantify non-economic losses like pain and suffering
- Track statute-of-limitations deadlines
- Represent you before an administrative law judge or in court
Your fight doesn’t stop at the denial notice. By combining regulatory complaints, external reviews, patient assistance programs, and legal counsel, you build a full-spectrum defense against unfair insurance tactics. Reach out to our Houston car accident lawyers for a free, no-obligation consultation.
When To Hire A Texas Injury Attorney
A crash can turn your world upside down in an instant. When your insurer keeps saying “no,” the stress mounts quickly. You deserve straightforward advice, not more runaround. That’s where a Texas injury attorney steps in—cutting through denials to protect your rights.
Signs You Need A Lawyer
Hitting the same roadblocks without progress? Watch for these red flags:
• Insurer has rejected your appeals more than twice without presenting new evidence
• Company delays payments or dangles lowball offers—classic bad faith tactics
• Medical bills exceed your policy limits with no reason given
• Ongoing disputes over liability or comparative fault percentages
These issues tie directly into Texas law: Chapter 33 of the Civil Practice & Remedies Code handles negligence, while Chapter 41 lets you pursue bad-faith claims against insurers.
Key takeaway A skilled attorney ensures you meet every deadline under the Chapter 16 statute of limitations.
Checklist Before Calling A Lawyer
If you check off two or more items below, it’s time for professional guidance:
• You’ve lost at least two internal appeals and nothing has changed in your policy
• Total medical or repair costs surpass $10,000
• Key evidence—police reports, expert opinions, etc.—is missing from your file
• The insurer won’t explain its denial or ignores your documentation
• Less than six months remain before the statute of limitations or appeal deadline
Don’t wait until you’ve exhausted every self-help option. Learn more in our detailed guide on when to hire a car accident lawyer.
How Attorneys Challenge Denials
Once you’re on board, your lawyer will:
• Scrutinize policy language and denial letters to pinpoint every error
• Use comparative fault analysis to shift blame and enhance your recovery
• Pursue pre-judgment interest in court to compensate for insurer delays
Common tactics include:
• Filing a tactical lawsuit to pressure a settlement in around 120 days
• Issuing a bad-faith demand under Chapter 541 of the Insurance Code
• Leveraging expert reports to rebut exclusions or damage caps
Next Steps With Your Attorney
In a free consultation, your attorney reviews denial letters and policy provisions line by line. You’ll explore mediation, bad-faith litigation, or filing suit before deadlines expire. Then you’ll receive a clear action plan to recover medical expenses, lost wages, and pain and suffering.
Real World Example
A Houston driver on I-45 faced repeated denials for necessary back surgery. Our team discovered missing X-ray records the insurer had overlooked. Within weeks, we secured a $45,000 settlement covering medical bills, lost wages, and pain and suffering. Acting swiftly made all the difference.
When To Reach Out
Insurance companies bank on delay. Missing a deadline is their strongest defense. A prompt call to The Law Office of Bryan Fagan stops that tactic cold.
You have nothing to lose with a free consultation—only clarity on your next steps. Contact The Law Office of Bryan Fagan today to discuss your rights and chart a path forward.
Frequently Asked Questions

You generally have 30 to 60 days from the date on your denial letter to file an internal appeal under Texas law. The moment that letter lands in your mailbox, set a reminder to protect your rights.
If two weeks pass and you’ve heard nothing, send a polite follow-up via certified mail or your insurer’s secure portal. Still no response? It’s time to file a complaint with the Texas Department of Insurance—an action that often prompts a mediator’s review.
Negotiation After Denial
Once your appeal period expires, you can begin negotiations. Lay out every cost—medical bills, repair estimates, lost wages—and propose a fair settlement.
- Itemize each loss with the date it occurred
- Label your documents clearly (for example, Repair Estimate 3/10/24)
- Always ask for a written counteroffer before agreeing
Potential Compensation
If your appeal is granted, you can recover:
- Medical expenses
- Vehicle repairs
- Lost income
- Non-economic damages (pain and suffering) under Texas Civil Practice & Remedies Code Chapter 41
Remember, Texas’s comparative-fault rules can adjust your award based on your share of responsibility.
Tips For Stronger Outcomes
- Keep a call and email log with timestamps
- Observe deadlines in Texas Insurance Code Chapter 542A for PIP claims
- Draft a concise evidence summary before mediation
Key Insight
Meticulous records and timely follow-up often turn initial denials into approvals.
Case Example
A Fort Worth driver had her PIP claim for a rental car rejected because the insurer claimed missing receipts. She filed a TDI complaint, highlighted the oversight, and within days received full rental reimbursement.
Tracking Deadlines And Documents
A simple calendar or color-coded spreadsheet keeps you on track. Note all critical dates: your appeal due date, the one-year window for TDI complaints, and the statute of limitations under Texas Civil Practice & Remedies Code Chapter 16.
- Record the denial date and appeal deadline
- Track the one-year TDI complaint deadline
Mediation As An Alternative
Mediation brings a neutral third party to help both sides reach agreement. It’s often quicker and less expensive than litigation. For help with auto insurance claim denials or wrongful death compensation, learn more about our car accident services.
Contact The Law Office of Bryan Fagan, PLLC for a free, no-obligation consultation at https://houstonaccidentlawyers.net








